California mental health services offer a comprehensive network of crisis support, treatment programs, and insurance-protected care for anyone struggling with mental health challenges or addiction. Whether you're in immediate crisis or seeking long-term treatment, the state provides multiple pathways to help.
Quick Access Guide:
Mental health is an essential part of healthcare, yet many Californians feel overwhelmed navigating the system. The truth is simple: if mental health or substance use is affecting your daily life, help exists near you.
California has transformed its behavioral health system through historic reforms. The Behavioral Health Services Act now addresses both mental health and substance use disorders together. This means better access to treatment, housing support, and crisis intervention across all 58 counties.
About 8% of Californians meet criteria for substance use disorder. Roughly 1 in 5 women and 1 in 7 men have experienced intimate partner violence. Around 25% of Americans grow up in homes where drug abuse is present. These statistics reveal a shared struggle—you're not alone.
The state offers everything from free digital mental health apps to residential treatment centers with evidence-based therapies like CBT, DBT, and EMDR. Whether you need a warm line for emotional support, medication management, or intensive dual diagnosis treatment for co-occurring conditions like depression and addiction, California's network can connect you to care.
This guide walks you through immediate crisis resources, insurance rights, treatment options, and specialized programs. You'll learn how to access county services, what to do if coverage is denied, and how residential programs support long-term recovery.
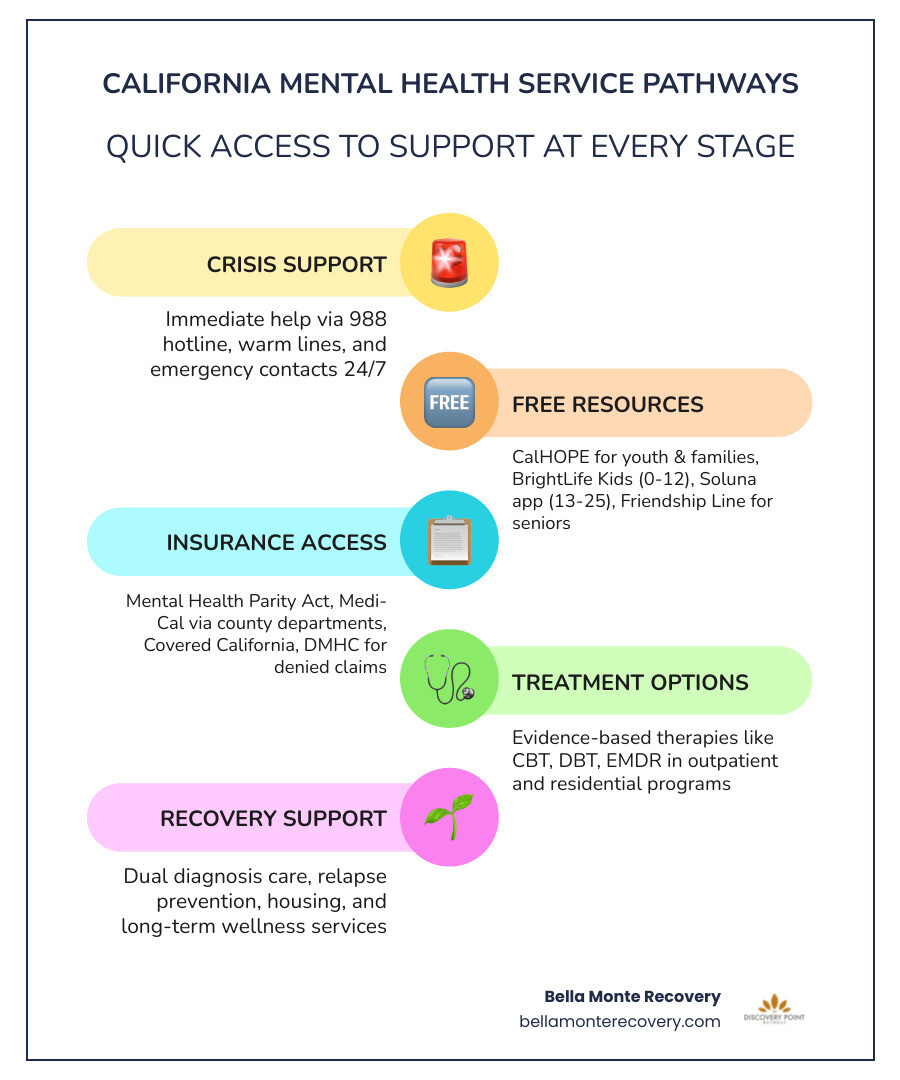
When you or someone you love is in the middle of a mental health emergency, every second counts. You don't have to figure it out alone. California has invested heavily in making sure help is just a phone call or text away, 24 hours a day.
The most vital tool in your toolkit is the 988 Lifeline. By calling or texting 988, you are connected to trained counselors who can provide immediate support for suicidal thoughts, substance use crises, or any other form of emotional distress. If you prefer typing over talking, you can talk to someone now through their online chat portal.

Beyond immediate life-threatening emergencies, we often need "warm" support—someone to talk to when we are stressed, anxious, or lonely but not necessarily in a life-threatening state. For this, California offers several specialized resources:
The state has recognized that children and young adults face unique pressures. To address this, California launched a groundbreaking program providing free, safe, and confidential digital mental health support.
Parents with children ages 0-12 can access free resources for kids through BrightLife Kids, which offers mental health coaching and resources to help navigate childhood behavioral challenges. For teens and young adults (ages 13-25), the Soluna app provides a private space for self-help tools, peer support, and professional coaching.
The CalHOPE Schools initiative further integrates these resources into the educational system, ensuring that teachers and administrators have the tools to support student wellness. This "mental health for all" approach ensures that regardless of income, California's youth have a fighting chance at a healthy future.
Understanding how to pay for or access care is often the biggest hurdle. In California, your rights to behavioral health care are protected by some of the strongest laws in the country.
The California Mental Health Parity Act, significantly amended in 2020, requires insurance companies to cover mental health and substance use disorders just as they would physical ailments. This means they cannot impose more restrictive co-pays, deductibles, or treatment limits on your mental health care than they do for a broken leg or a heart condition.
If you are a member of a commercial health plan, you have specific member rights. These include:
For those without private insurance, Covered California provides a gateway to affordable plans that include essential behavioral health benefits. If you have coverage but are facing a denial of service, the Department of Managed Health Care (DMHC) ombudsman is there to help you file a grievance and ensure you get the care you are legally owed.
Accessing California mental health services through Medi-Cal involves working with your local county mental health department. These departments are responsible for providing "specialty mental health services" for individuals with significant functional impairments.
To start the process:
The state also supports primary care providers through Cal-MAP, a consultation service that helps doctors manage their patients' mental health needs more effectively within a primary care setting.
Parity laws have revolutionized how we treat conditions like PTSD and depression. Historically, insurance might have limited you to a handful of therapy sessions per year. Under current laws, treatment must be based on medical necessity, not arbitrary caps.
This legal framework encourages the use of evidence-based modalities—treatments that have been scientifically proven to work. Whether you are seeking help for navigating dual diagnosis (having both a mental health and substance use disorder) or looking for specialized trauma care, parity ensures your insurance is a tool for recovery, not a barrier.
At Bella Monte Recovery, we believe that true healing requires a blend of modern science and holistic wellness. California’s top treatment centers have moved away from "cookie-cutter" approaches, instead opting for individualized care plans that treat the whole person.
Beyond talk therapy, holistic addiction treatment incorporates the mind-body connection. This might include:
Whether you are seeking OCD treatment or help with a complex mood disorder, these combined therapies provide a robust foundation for change.
For many, a "serene environment" is the catalyst for a breakthrough. Residential treatment offers 24/7 care in a safe, home-like setting, away from the triggers of daily life. This is especially vital for Dual Diagnosis—when a person struggles with both addiction and a condition like depression.
Residential programs in Southern California, like those in Desert Hot Springs, often feature low client ratios. This ensures that every individual receives the personalized attention they need. During depression rehab, patients learn relapse prevention skills and receive bipolar support if needed, all while surrounded by the natural beauty of the California desert.
Addiction is a chronic illness, not a moral failing. In California, we are seeing a shift toward treating Substance Use Disorders (SUD) with the same medical rigor as diabetes or heart disease.
For severe conditions like schizophrenia, California's network of county services and private residential centers provide stabilization, medication management, and long-term support. Neurotherapy and medically supervised detoxification are also available to ensure the transition into sobriety is as safe and comfortable as possible.
If your insurance denies care, do not give up. First, contact your health plan’s member services and file a formal grievance. If they do not resolve the issue within 30 days (or 3 days for urgent cases), contact the DMHC Help Center at 1-888-466-2219. You may be eligible for an Independent Medical Review (IMR), where an outside doctor reviews your case. California law requires plans to provide "timely access" to care; if they can't find an in-network provider quickly, they must pay for an out-of-network one.
The Behavioral Health Services Act (BHSA) is a modern evolution of the 2004 Mental Health Services Act (MHSA). While the MHSA focused primarily on mental health, the BHSA expands the scope to include Substance Use Disorder (SUD) treatment. It also prioritizes housing interventions for those with the most severe needs and expands the behavioral health workforce. It brings enhanced oversight and accountability to ensure that the 1% tax on millionaires is being used effectively to reduce homelessness and provide equitable care.
California has 21 Regional Centers that serve individuals with developmental disabilities that began before age 18 (such as autism, cerebral palsy, or intellectual disabilities). These centers provide a statewide network of support, including early intervention for infants, behavioral health services, and coordination of care. They are a vital resource for families navigating the intersection of developmental needs and mental health.
Navigating California mental health and addiction services can feel like a daunting journey, but the resources available today are more robust and compassionate than ever before. From the immediate support of the 988 lifeline to the long-term healing found in residential care, you are supported at every step.
At Bella Monte Recovery, we specialize in providing Desert Hot Springs Dual Diagnosis care that addresses the whole person. Our personalized, evidence-based addiction and mental health treatment plans are designed to help you reclaim your life in a serene, supportive environment. Whether you are dealing with depression, anxiety, or a complex substance use disorder, our team is dedicated to your transformative care.
Don't wait for a crisis to reach out. Whether for yourself or a loved one, the path to a brighter, healthier future is open. Start your journey to recovery today and discover the difference that compassionate, expert care can make.
Group therapy sessions are a powerful form of treatment where 5-15 people meet regularly with one or two trained therapists to share experiences, learn coping strategies, and support each other's recovery. If you're considering this option, here's what you need to know:
Quick Overview of Group Therapy Sessions:
Imagine walking into a room full of strangers and being asked to share your deepest struggles. For most people entering treatment, this feels intimidating—even terrifying. But here's what research shows: those same people often describe group therapy as the most valuable part of their recovery journey.
You're not alone in feeling isolated by addiction or mental health challenges. That sense of being the only one struggling is part of what keeps people stuck. Group therapy sessions break that isolation by creating a circle of support where you realize others understand exactly what you're going through.
The evidence is clear. Studies show group therapy produces outcomes comparable to individual therapy for conditions including depression, PTSD, anxiety disorders, substance use disorders, and more. It works because humans are wired to heal in community—we learn, grow, and change more effectively when we're not doing it alone.
At its core, group therapy offers something individual sessions cannot: the power of shared experience, the validation of being truly understood, and the opportunity to both receive and give support.

At its most basic level, group therapy is a form of psychotherapy where a trained professional works with several people at once. It isn't just a "chat group" or an informal support meeting; it is a structured clinical intervention designed to help you achieve specific mental health or recovery goals.
The logistics are fairly straightforward. Most group therapy sessions consist of 5 to 15 members, though the "sweet spot" for many clinicians is between 7 and 10 participants. This size ensures there are enough voices to provide diverse perspectives, but not so many that anyone gets lost in the crowd. Sessions typically last between 60 and 120 minutes, giving everyone a chance to participate.
One of the most important things to understand is that group therapy is an evidence-based specialty. According to research on group therapy effectiveness, this approach is just as effective as individual counseling for a wide range of conditions. In some cases, such as substance use recovery or social anxiety, it can actually be more effective because of the peer-to-peer accountability and social modeling it provides.
| Feature | Individual Therapy | Group Therapy |
|---|---|---|
| Focus | One-on-one attention on personal history | Interpersonal dynamics and shared experiences |
| Perspective | Therapist's professional insight | Diverse insights from peers and therapist |
| Social Environment | Private and isolated | Microcosm of the real world |
| Cost | Typically higher | Generally more cost-effective |
| Primary Benefit | Deep dive into individual trauma | Breaking isolation and practicing social skills |
While individual therapy provides a safe space for a deep dive into your personal history and private thoughts, group therapy offers something different: an interpersonal microcosm.
In a one-on-one session, you talk about your relationships. In a group session, you live them. The group becomes a mini-version of the outside world. If you struggle with authority, those feelings will likely come up with the therapist. If you struggle with people-pleasing, you’ll likely find yourself doing it with other members. This allows the therapist to observe these behaviors in real-time and offer immediate, gentle feedback.
Furthermore, the "peer feedback" element is unique. Hearing a therapist say you're being too hard on yourself is one thing; hearing it from five other people who are "in the same boat" often carries a different kind of weight. It feels less like clinical advice and more like a shared truth.
Group therapy is a versatile tool. It is highly suitable for individuals dealing with:
If you want to dive deeper into how these sessions are structured, you can find more info about group therapy on our specialized service page.
The magic of group therapy sessions lies in the "therapeutic factors" first identified by Dr. Irvin Yalom. The most immediate benefit is universality—the "same boat" feeling. When you struggle with mental health or addiction, you often feel like a "broken" exception to the rest of the world. In a group, you see your struggles mirrored in others, which instantly lowers your defenses.
Another profound benefit is altruism. In individual therapy, you are always the recipient of help. In a group, you have the opportunity to offer a kind word, a shared insight, or a supportive nod to someone else. This boosts your sense of self-worth and reminds you that you still have value to give, even when you’re hurting.
For those in the early stages of change, the benefits of group therapy in addiction recovery are particularly strong. You get to see "social modeling" in action—watching peers who are further along in their journey successfully navigate challenges provides a roadmap for your own success.
Addiction thrives in the dark. It wants you alone, ashamed, and disconnected. Group therapy sessions pull you into the light.
Emotional resilience is like a muscle; you have to flex it to make it stronger. Group therapy provides a "safe gym" for this. Through catharsis—the honest, sometimes raw expression of suppressed emotions—you learn that feelings won't kill you.
In these sessions, we often utilize evidence-based tools. For instance, you might learn Dialectical Behavior Therapy (DBT) skills to manage intense emotions. Instead of acting out on a feeling, you learn to observe it, name it, and discuss it with the group. This "interpersonal learning" is what builds the hope necessary to keep moving forward.
Not all groups are the same. Depending on your needs, you might participate in different formats:
Skill-based groups are highly structured and focused on giving you "tools for your belt." We often incorporate Cognitive Behavioral Therapy (CBT) strategies to help you identify the "stinking thinking" that leads to negative emotions.
You might also explore:
These groups focus on the "feedback loops" of human interaction. If you have a habit of interrupting people when you're anxious, someone in the group will eventually point it out. Because the environment is supportive, you can hear that feedback without feeling attacked. You can then try out a new behavior—like active listening—and get immediate positive reinforcement. This helps resolve long-standing childhood patterns of communication that may no longer serve you.
You don't just "show up" to a group. There is a process to ensure the group is a good fit for you and you are a good fit for the group.
Every group goes through a predictable lifecycle, often described as:
The therapist isn't just a bystander; they have several critical "executive functions." They set the boundaries, ensure the room stays safe, and manage the "group anxieties."
They also facilitate "meaning-attribution"—helping you connect the dots between what's happening in the group and what's happening in your life. Research shows that a strong therapeutic alliance between the facilitator and the members is one of the best predictors of a positive outcome. They are the "guardians of the safety zone," making sure that feedback remains constructive and that everyone follows the confidentiality rules.
Yes. Extensive research on group vs. individual counseling confirms that group therapy is a highly effective, evidence-based treatment. For many conditions, including anxiety and substance use, the outcomes are virtually identical. In fact, because groups offer peer support and social modeling, some people find they make progress faster in a group setting than they do alone. It also provides a more cost-effective way to access high-quality professional care.
Absolutely. This is often called "combined" or "conjoined" therapy. Many of our clients find that individual therapy sessions allow them to process deep trauma, while group sessions allow them to practice the social skills and emotional regulation they discuss in private. This "double-dose" of support can significantly accelerate your recovery.
Confidentiality is the cornerstone of any group therapy session. Before joining, every member must sign a formal agreement promising not to share the names or stories of other participants outside the room. While a therapist is legally bound by HIPAA, group members are ethically bound by the "contract" they make with each other. We find that because everyone in the circle wants their own privacy respected, they are incredibly protective of the privacy of others. For more technical details, you can look into research on confidentiality in group psychotherapy.
Healing doesn't happen in a vacuum. It happens in the presence of others who see us, hear us, and walk beside us. At Bella Monte Recovery Center, we believe in a holistic, personalized approach to recovery. Whether you are struggling with depression, anxiety, or addiction, our group therapy sessions in Desert Hot Springs provide the community you need to thrive.
You don't have to carry the weight of the world on your own shoulders. By joining a circle of support, you gain the strength of the entire group. If you're ready to break the cycle of isolation and start a new chapter, we are here to help.
Take the first step toward a brighter, more connected future. Start your recovery journey in Palm Springs with us today and discover the power of healing together.
10 coping skills for addiction recovery are practical tools that help you manage cravings, avoid triggers, and build a life beyond substance use. Here are the essential skills you need:
One of the hardest parts about getting sober is learning how to cope with all the stress life throws at you without using drugs or alcohol. As one person in recovery put it: "If I just make it to bed I'll be fine. Sometimes it's just for the next 30 minutes or even the next 30 seconds."
Addiction often develops when we use substances as maladaptive coping mechanisms to deal with stress, trauma, or difficult emotions. The brain's reward system becomes hijacked, making substances feel like the only solution to life's problems.
The cycle of addiction has three stages: active use, withdrawal, and relapse. Without healthy coping skills, this cycle repeats itself. More than two-thirds of patients relapse within weeks to months after treatment, with relapse rates for substance use disorders ranging from 40% to 60%.
But here's the good news: developing healthy coping skills can interrupt this cycle. These tools help you manage the root causes of addiction—whether that's anxiety, loneliness, or past trauma—without turning to substances.
Relapse itself happens in stages. First comes emotional relapse (negative thoughts and isolation), then mental relapse (considering use), and finally physical relapse (actual use). Learning to recognize and respond to these stages early is key to maintaining your recovery.
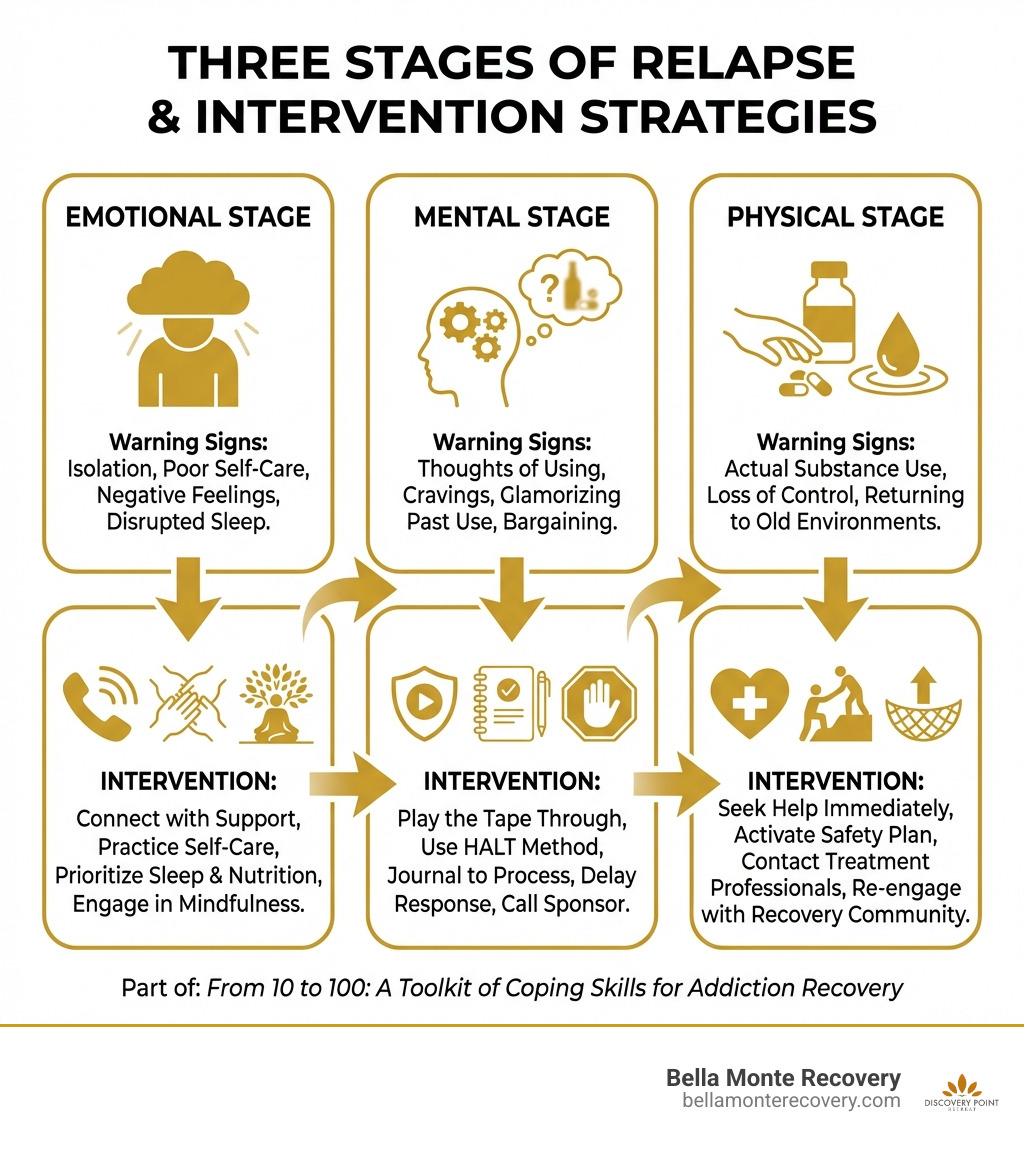
To understand why these skills are so vital, we have to look at what addiction does to the brain. Drugs and alcohol hijack the brain’s reward center, releasing massive amounts of dopamine. This is the chemical that regulates pleasure. Over time, the brain becomes resistant to dopamine’s effects, making it harder to feel joy from normal activities. This "hijacking" makes solo coping incredibly difficult because your brain is literally telling you that you need the substance to survive.
Scientific research on healthy coping skills shows that learning to deal with stress and negative emotions is one of the four tenets of successful relapse prevention. By implementing these skills, we aren't just "stopping" a bad habit; we are relearning how to be human. We are training the brain to find balance again.
At Bella Monte Recovery, we focus on the dangers of relapse and how to prevent it by providing a toolkit that addresses the whole person. Coping skills act as a circuit breaker. When a trigger occurs, the skill interrupts the automatic path toward use and provides a different, healthier exit ramp.
Before we can use our skills, we have to know what we are up against. Triggers are the "red flags" that signal a craving might be coming. They generally fall into two categories:
Common triggers for relapse often include financial pressure or work stress. By recognizing your trauma triggers to prevent relapse, you can prepare an action plan before the emotions become overwhelming. We often suggest our clients keep a list of these triggers so they aren't caught off guard. When you know that a certain family member always makes you feel anxious, you can plan to use a specific coping skill before you even walk into the room. For more on this, check out our guide on triggers and coping strategies in recovery.
Cravings are a normal part of the process. They are not a sign of failure; they are a sign of healing. Most cravings actually end within an hour, which means you don't have to fight them forever—you just have to outlast them.
One powerful technique is "Urge Surfing." Imagine the craving is a wave. If you try to block it, it will knock you over. If you "surf" it—observing the physical sensations without acting on them—the wave eventually crests and washes away.
Impulsivity is a hallmark of substance use disorders because the brain's area for regulating impulse control has been affected. To combat this, we use the HALT method. This is a quick self-check to see if your physical needs are being met, which often reduces the intensity of the urge.
| HALT Symptom | Immediate Solution |
|---|---|
| Hungry | Eat a nutritious snack or meal. Low blood sugar mimics anxiety. |
| Angry | Practice deep breathing or call a sponsor to vent. |
| Lonely | Reach out to a friend or go to a meeting. Isolation feeds addiction. |
| Tired | Take a nap or commit to an early bedtime. Exhaustion lowers defenses. |
Research on mindfulness for relapse prevention shows that these practices improve quality of life and significantly reduce anxiety. Mindfulness isn't about clearing your mind; it's about non-judgmental and non-reactive awareness. You notice the thought "I want to drink," and instead of panicking, you say, "I am having a thought about drinking," and let it pass. This is why mindfulness is essential for long-term healing.
As mentioned above, checking in on your basic needs is a primary defense. We often forget that something as simple as being dehydrated or needing a sandwich can feel like a spiritual crisis when you're in early recovery.
This is a core Cognitive Behavioral Therapy (CBT) technique. When you have a "romantic" thought about using (euphoric recall), stop and play the tape to the end. Don't just think about the first five minutes; think about the inevitable crash, the shame, the lost money, and the pain caused to loved ones. This technique is vital for predicting treatment outcomes because it forces the logical brain to take over.
Exercise is a double-win. First, it activates the brain’s reward system naturally, helping to restore dopamine levels. Second, it reduces the stress that often leads to relapse. Whether it's a walk in the Palm Springs sun or adventure therapy and how it aids in addiction recovery, moving your body is medicine.
Sometimes feelings are too big for words. How art therapy aids in addiction recovery is by allowing you to externalize what’s inside. Journaling works similarly; it helps with making plans and managing negative emotions. If you're stuck, try addiction recovery journal prompts to get the ink flowing.
You cannot do this alone. Studies show that social support can foster self-efficacy and reduce cravings. Whether it's a 12-step group or a secular community, having people to call when things get tough is non-negotiable. Are support groups important in recovery? Absolutely. They provide the accountability you need when your own will feels weak.
Impulsivity is a hallmark of substance use disorders. When you feel an urge or get angry, commit to waiting just 15 minutes before taking any action. Usually, the intensity of the emotion will drop significantly in that window.
Sleeplessness is a common symptom of withdrawal. However, the brain needs sleep to learn new habits after recovery. Aim for 7 to 9 hours of sleep per night. A rested brain is a resilient brain. Is sleep important in recovery? It is the foundation of your mental health.
Self-care isn't just bubble baths. It’s practising good oral health, attending doctor appointments, and eating well. These habits improve emotional resilience and remind you that you are worth looking after.
Acts of kindness are linked to lower inflammation and can even impact levels of inflammation in the body. Helping a newcomer at a meeting or volunteering takes the focus off your own cravings and gives you a sense of purpose.
While self-help tools are incredible, some roots go too deep to pull alone. Professional therapy provides a safe space to develop these 10 coping skills for addiction recovery under the guidance of experts.
The therapeutic alliance—the relationship between you and your therapist—is one of the strongest predictors of success. In a clinical setting, you can practice these skills in real-time, receiving feedback and adjustments. The power of therapy in rehabilitation lies in its ability to build a foundation that lasts long after you leave our Desert Hot Springs facility.
Many people struggling with addiction also deal with a "dual diagnosis," such as depression or PTSD. In these cases, standard coping skills might need a boost from specialized therapies:
By combining these professional interventions, you aren't just surviving; you're thriving. You're building a "toolkit" that is personalized to your specific history and needs.
First, breathe. Relapse is often a part of the recovery process, not the end of it. The relapse rate for substance use is similar to other chronic illnesses like asthma (50% to 70%). If it happens, be honest with your support network immediately. Analyze what happened: was there a trigger you missed? Did you stop using your daily skills? Use it as a learning opportunity to strengthen your Aftercare Program.
Research shows that most intense cravings end within an hour. While they feel like they will last forever, they are temporary. Using "distraction" skills—like calling a friend, going for a walk, or doing a puzzle—can help you bridge that 60-minute gap.
Lying is a common habit during active addiction. In recovery, honesty is a protective shield. When you are honest about your cravings, they lose their power. Secrets grow in the dark; honesty brings them into the light where they can be managed.
Building a toolkit of 10 coping skills for addiction recovery is a lifelong journey. At Bella Monte Recovery Center in Southern California, we believe in a personalized, whole-person approach. Whether you are in Palm Springs or Desert Hot Springs, our mission is to help you reclaim your life through evidence-based care and compassionate support.
Recovery isn't just about what you're leaving behind; it's about the beautiful life you're creating. By staying active in your Aftercare Program and consistently practicing these skills, you can maintain long-term sobriety and find a sense of peace you never thought possible.
If you or a loved one is struggling, you don't have to walk this path alone. Reach out today, and let's start building your toolkit together.
Drug addiction triggers are stimuli—people, places, emotions, or situations—that activate intense cravings and can lead to relapse. Research shows that up to 40-60% of people in recovery experience relapse, making trigger identification and management essential for long-term sobriety.
Quick Guide to Drug Addiction Triggers:
Recovery from addiction is challenging because your brain has been fundamentally changed by substance use. Even after you stop using, those neurological pathways remain—waiting to be activated by the right trigger. A familiar smell, a stressful day at work, or driving past an old hangout can instantly flood your brain with cravings.
But here's the important part: triggers don't have to lead to relapse. When you understand what triggers are, how they work, and why they're so powerful, you gain the knowledge needed to protect your sobriety. This guide will help you identify your personal triggers, understand the science behind them, and develop practical strategies to manage them effectively.
Whether you're just beginning recovery or working to maintain years of sobriety, learning to navigate triggers is one of the most valuable skills you can develop.
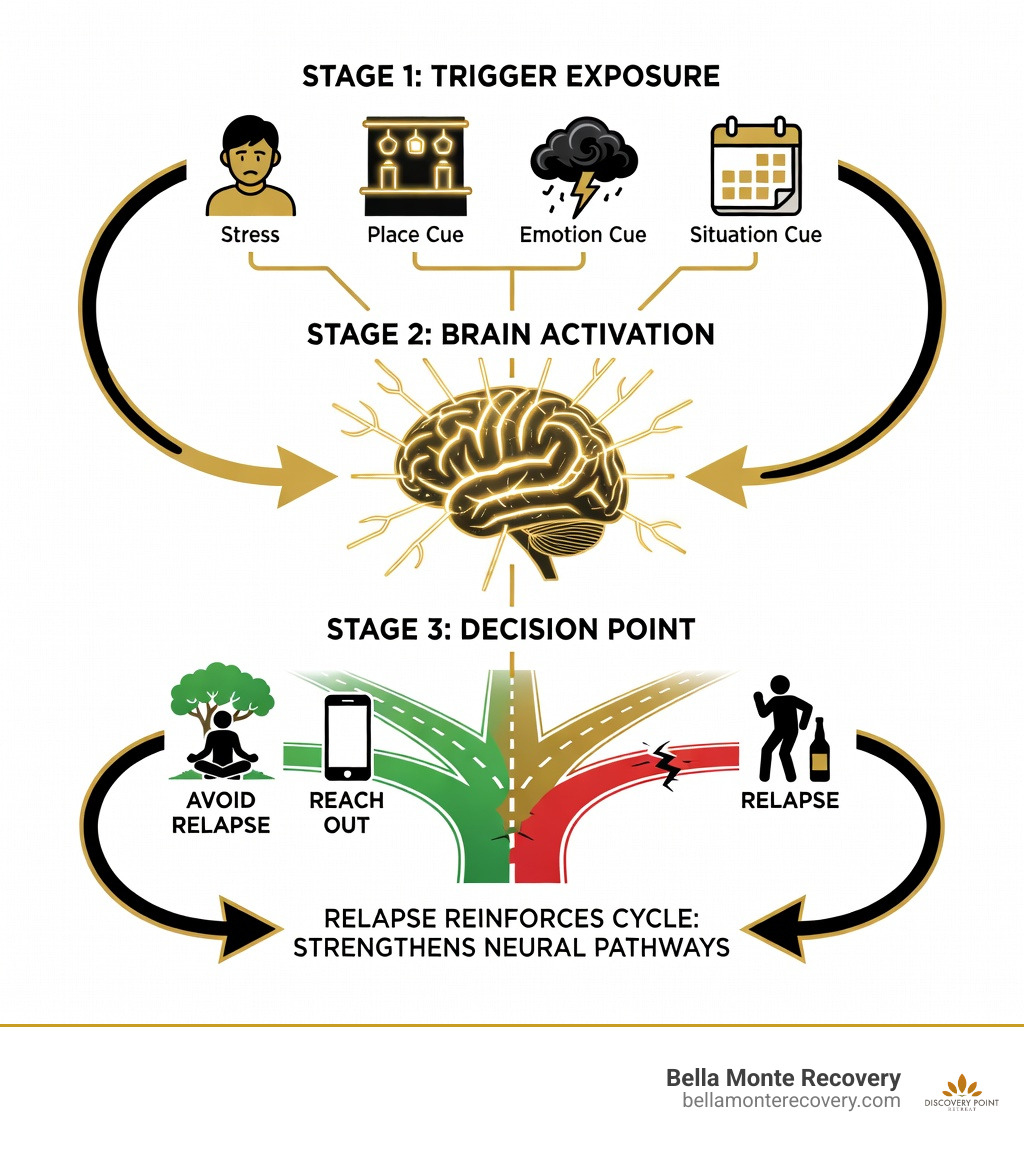
To effectively manage our recovery, we first need to understand exactly what we are up against. In the simplest terms, a trigger is a stimulus that elicits a reaction. In the context of substance use disorder, it is a psychological or environmental cue that initiates a craving response related to memories of drug or alcohol use.
Addiction is a chronic brain disease, not a moral failing. When we use substances, our brain's reward system is "hijacked." According to Scientific research on the neurobiology of addiction, the process involves a three-stage cycle:
Because of neuroplasticity, our brains are incredibly good at making associations. If we always used drugs in a specific park or with a specific friend, our brain wires those things together. Eventually, just seeing that park or friend can cause a subconscious dopamine release. This creates "incentive salience," where the brain anticipates a reward before we even consciously think about the substance. This is why triggers are so powerful; they often hit us before we realize what is happening.
| Feature | Drug Addiction Triggers | Cravings |
|---|---|---|
| Definition | The "spark" or cue (person, place, or feeling) | The "fire" or intense physical/emotional urge to use |
| Nature | Usually an external or internal event | A physiological and psychological state |
| Duration | Can be instantaneous | Can last minutes to hours (though they are temporary) |
| Control | Often avoidable or manageable through planning | Managed through coping skills and "riding the wave" |
Identifying your personal drug addiction triggers is like creating a map of a minefield. Once you know where the mines are buried, you can walk around them. Identification often begins during professional treatment, where we work with counselors to look back at our history and pinpoint exactly what led to past use.
We generally divide triggers into two categories: external and internal.
Internal triggers are often the most difficult to manage because we cannot simply walk away from our own feelings. They require emotional awareness and regulation.
External triggers are often powerful but, in many cases, they are avoidable. By changing our environment and social circles, we can significantly reduce the number of cues we encounter daily.
Relapse is rarely a sudden event. It is a process that often begins weeks or months before the actual physical act of using. Understanding the stages—emotional, mental, and physical relapse—helps us intervene early.
Stress is perhaps the most universal trigger. When we are stressed, our bodies release cortisol. For someone in recovery, high cortisol levels can weaken the prefrontal cortex (the "Stop" system) and strengthen the "Go" system of the basal ganglia. This creates a biological "perfect storm" for relapse. Whether it is financial pressure, work stress, or social anxiety, learning to manage stress without substances is a cornerstone of recovery.
Certain situations increase the likelihood of encountering drug addiction triggers:
While avoiding triggers is the first line of defense, we cannot avoid life forever. We need a toolkit of coping mechanisms to use when a trigger is unavoidable.
Building a "sober life" that you actually enjoy is the best way to prevent relapse.
If you do experience a relapse, it is vital to remember that you have not "failed." Because addiction is a chronic illness, relapse is often a sign that the treatment plan needs to be adjusted.
Think of a trigger as the "match" and a craving as the "flame." A trigger is an event or feeling that happens first. It then sets off a craving—the actual physical or mental urge to use. You can often avoid the "match," but once the "flame" starts, you need coping skills to put it out.
While you can eliminate many external triggers (by changing your phone number, moving, or finding new friends), internal triggers like stress and sadness are part of the human experience. The goal of recovery isn't to live a life without triggers, but to become so resilient that they no longer have power over you.
First, remove yourself from the situation if possible. Then, use a grounding technique: breathe deeply, name five things you see, and call a member of your support system. Remind yourself that the craving is a temporary chemical reaction in your brain that will pass if you wait it out.
Navigating drug addiction triggers is a lifelong journey, but it is one you don't have to take alone. By understanding the neurobiology of how our brains respond to cues, we can move from a place of fear to a place of empowerment. Recovery isn't about willpower; it's about having a solid plan, a strong support network, and the right professional guidance.
At Bella Monte Recovery Center, we understand that every individual's journey is unique. We offer personalized, evidence-based addiction and mental health treatment in the serene environment of Desert Hot Springs. Our comprehensive, holistic recovery plans address the root causes of addiction, including co-occurring issues like depression and anxiety.
Whether you are in Palm Springs, Southern California, or anywhere else in the state, we are here to help you reclaim your life. If you or a loved one is struggling, relapse is not the end—it's an opportunity to strengthen your recovery.
Begin your recovery journey today and discover the tools you need for a lasting, sober future.
The 5 stages of trauma healing provide a roadmap for understanding how people move from the immediate shock of a traumatic event toward lasting recovery and growth. Here's what the journey typically looks like:
Recovering from a traumatic event often feels like navigating a maze without a map. You might feel stuck, overwhelmed, or unsure if you're making any progress at all.
Here's what matters: 70% of U.S. adults will experience a traumatic event at least once in their lives. You're not alone in this struggle.
The stages of trauma healing aren't a straight line. You might move forward, then slide back. You might spend months in one stage and weeks in another. Some days you'll feel like you're healing, and other days the pain feels as fresh as it did on day one.
But understanding these stages changes everything. When you know where you are in the journey, you can stop wondering "What's wrong with me?" and start asking "What do I need right now?"
Trauma doesn't just live in your mind—it gets trapped in your body. Your nervous system stays on high alert. Your muscles hold tension. Research shows that people with PTSD report significantly higher rates of chronic pain, digestive issues, and persistent fatigue compared to those without trauma histories.
This guide will walk you through each stage of trauma healing, explain what's happening in your brain and body, and give you practical strategies to move forward. Whether you're just beginning to acknowledge your trauma or you're years into your recovery, understanding this roadmap can help you find your way to emotional freedom.

To understand the 5 stages of trauma healing, we first have to understand why we feel "stuck" in the first place. It isn't a lack of willpower; it’s biology.
When we experience a traumatic event—whether it’s a single accident or years of complex emotional abuse—our brain’s "alarm system" takes over.
During trauma, the amygdala (the brain's emotional smoke detector) becomes hyper-reactive. It sends out a frantic "fight-or-flight" signal to the rest of the body. Meanwhile, the prefrontal cortex—the part of the brain responsible for logic, language, and time-stamping memories—effectively goes offline.
Because the prefrontal cortex isn't working correctly, the brain fails to file the memory as "past history." Instead, the trauma stays "live." This is why scientific research on the neurobiology of emotional trauma suggests that trauma causes lasting changes in how the brain handles stress.
Trauma isn't just a mental event; it’s a physical one. When the nervous system gets stuck in a state of high arousal, it manifests as physical symptoms. Research from the American Psychological Association on chronic stress shows that emotional trauma contributes to high blood pressure, heart disease, autoimmune disorders, and chronic pain.
Your body remembers what your mind may be trying to forget. This "body memory" is why you might feel a sudden surge of panic or physical pain without knowing why—your nervous system has spotted a "trigger" that reminds it of the original trauma.
Healing is rarely a straight line. Think of it more like a winding mountain path. You might feel like you’ve reached a peak, only to find yourself back in a valley the next day. This is normal.
The 5 stages of trauma healing are often compared to the Kübler-Ross grief model (Denial, Anger, Bargaining, Depression, Acceptance). While they share similarities—because trauma always involves the loss of safety or innocence—trauma recovery has its own unique hurdles. Studies published in the Journal of Traumatic Stress on trauma and chronic pain emphasize that healing requires addressing both the mind and the physical body simultaneously.
To help navigate this, many experts point to the "5 R’s of Trauma":
The first two stages are all about survival.
Stage 1: The Emergency/Impact Stage
This is the immediate aftermath. You are in shock. Your brain is flooded with cortisol and adrenaline. You might feel disoriented, shaky, or completely "out of it." In this stage, the goal isn't "healing"—it's simply finding safety. If you are in Southern California and experiencing this, your priority is securing a safe environment and meeting basic needs like sleep and hydration.
Stage 2: The Denial/Numbing Stage
Once the immediate shock wears off, your brain may try to protect you by numbing your emotions. This is a form of cognitive dissonance. You might tell yourself, "It wasn't that bad," or "Other people have it worse."
While denial serves as a temporary shield, staying here too long prevents the processing of the event. Common behaviors in this stage include:
As the "numbness" wears off, the trauma often begins to intrude on your daily life. This is frequently the most difficult part of the 5 stages of trauma healing.
In the Intrusive Stage, the memories that were suppressed start to leak out. You might experience flashbacks, where it feels like the event is happening all over again. Nightmares, hypervigilance (constantly scanning for danger), and sudden panic attacks are common.
This is the stage where many people feel "broken," but it is actually a sign that your brain is trying to process what happened. The challenge is moving from dysfunctional coping to healthy regulation.
| Dysfunctional Coping | Healthy Coping Mechanisms |
|---|---|
| Substance abuse to "black out" memories | Grounding techniques (5-4-3-2-1) |
| Total isolation from loved ones | Reaching out to a trusted support system |
| Self-blame and "bargaining" | Self-compassion and trauma education |
| Suppressing anger until it explodes | Expressing anger through exercise or art |
Breaking the silence is a key part of this stage. Whether it’s telling a therapist or a close friend, bringing the trauma into the light reduces its power.
These stages represent the shift from "surviving" to "thriving."
Stage 4: The Transition/Integration Stage
In this stage, you stop fighting the reality of what happened. You move into active acceptance. You might start a professional recovery program or begin specialized therapies like EMDR. You start to reconstruct your personal narrative—moving from "victim" to "survivor."
Stage 5: Long-Term Recovery and Reconstruction
This isn't about the total absence of symptoms; it's about management and growth. You have a "toolbox" of coping skills. You can think about the past without your heart racing. Research on CBT and EMDR effectiveness for PTSD shows that these evidence-based treatments significantly reduce symptoms, allowing for a "new normal."
In this final stage, many people experience post-traumatic growth, where they find new meaning and strength they didn't know they had.
Because trauma lives in the body, talk therapy is often not enough on its own. We need to "speak" to the nervous system.
There is a concept in psychology called the Judith Herman model, which emphasizes that the final stage of recovery is "Reconnection."
Post-traumatic growth is the highest stage of the recovery roadmap. It doesn't mean you're glad the trauma happened—it means you have integrated the experience into your life in a way that produces:
There is no "standard" timeline. For some, the journey takes months; for others, it takes years. Factors like the duration of the trauma, your support system, and whether you seek professional help all influence the timeline. The goal is progress, not speed.
Absolutely. Healing is non-linear. A new stressor or a "trauma anniversary" might pull you back from Stage 5 to Stage 3. This isn't a failure; it's a normal part of the process. Each time you revisit a stage, you do so with more tools and wisdom than before.
Grief is the response to loss; trauma is the response to a threat to your safety or life. While they overlap (especially in the Denial and Depression phases), trauma recovery requires specific focus on the nervous system and the "fight-or-flight" response, which grief models don't always address.
If you feel stuck in the intrusive or numbing stages of your journey, please know that professional support can make the difference between "treading water" and actually moving forward.
At Bella Monte Recovery, we specialize in helping individuals navigate the 5 stages of trauma healing through a personalized, holistic approach. Whether you are dealing with a single-event trauma or complex, long-term issues, our team in Desert Hot Springs is here to help you reclaim your life.
We provide comprehensive care, including more info about dual diagnosis services for those who have turned to substances to cope with their pain. You don't have to walk this path alone. Sustainable recovery is possible, and your journey toward emotional freedom can start today.
Xanax (alprazolam) is a prescription benzodiazepine commonly used to treat anxiety and panic disorders. But like all medications, it comes with potential side effects. While some users experience mild issues like drowsiness or dizziness, others may face more serious risks such as dependency, withdrawal symptoms, or cognitive impairment.
In this article, we will cover the full range of Xanax side effects, both short-term and long-term, so you can make informed decisions about your treatment and stay safe.
Xanax1, known generically as alprazolam, is a type of medication called benzodiazepines, which act as a central nervous system depressant. It primarily alleviates symptoms of anxiety and panic disorders, providing calm and reducing the severity of panic attacks.
This medication is a cornerstone in treating anxiety disorders, making it a vital tool for many individuals seeking relief from overwhelming stress and anxiety.
Xanax is available as standard tablets, extended-release tablets, and orally disintegrating tablets, each designed to meet various treatment needs.
Following the prescribed dose meticulously helps avoid complications. Misuse or overuse can lead to severe consequences like xanax overdose and an unusual sense of mental and physical coordination. Approaching this medication with caution under strict healthcare provider guidance is vital.

While Xanax can be a lifeline for those with anxiety disorders, it comes with a roster of common side effects that users should be aware of2.
These include:
These side effects of taking alprazolam can significantly impact an individual’s daily life. For instance, they might make it challenging to perform routine tasks, leading to a decrease in productivity and an increase in frustration.
These symptoms can be particularly bothersome and interfere with one’s quality of life, making it imperative to manage them properly.
Consult a healthcare professional for management strategies if these side effects occur. Promptly addressing these adverse effects can prevent escalation and ensure safer treatment.
While the common side effects of Xanax can be managed with proper care, some severe side effects require immediate medical attention. Taking large doses of alprazolam can result in strong depressive effects1. It can also cause memory problems. These symptoms can be life-threatening, necessitating urgent intervention to prevent further complications.
One of the gravest risks associated with Xanax is the presence of counterfeit pills, which may contain dangerous substances like methamphetamine or fentanyl3. These counterfeit pills significantly increase health risks, leading to severe adverse effects and even death. Obtaining Xanax from reputable sources and ensuring its authenticity is crucial.
In the event of a Xanax overdose, monitoring vital signs like respiration, blood pressure, and pulse rate, including deep or fast breathing, is critical. Immediate medical attention is essential for managing these severe side effects and ensuring patient safety.

Long-term use of Xanax4 brings with it the risk of developing physical dependence. Regular use, even under healthcare supervision, can lead to significant physical dependence, making withdrawal challenging. The effects of alprazolam, such as disinhibition and euphoria, contribute to its potential for misuse and addiction.
Chronic treatment with high daily doses increases the risk of dependence and difficult withdrawal symptoms. Abruptly stopping the medication can result in severe withdrawal symptoms, including convulsions, muscle cramps, and unusual behavior. These symptoms can worsen significantly if not managed properly, leading to potentially dangerous complications.
Tapering off Xanax gradually under medical supervision mitigates these risks. This method manages withdrawal symptoms effectively and reduces severe adverse effects. Professional help is crucial if dependence signs or worsening withdrawal symptoms appear.
Knowing the differences between immediate-release and extended-release tablets is key to managing alprazolam tablets’ effects. Immediate-release tablets provide rapid relief from anxiety symptoms by releasing the medication quickly. This can be particularly beneficial during acute anxiety attacks requiring immediate intervention.
Extended-release tablets release the medication gradually over a longer duration, providing prolonged effects. This maintains more stable blood levels, reducing the peaks and troughs of immediate-release forms. An extended release tablet may offer a more consistent and manageable approach to treating anxiety and panic disorders.
Mixing Xanax, a benzodiazepine, with other substances, particularly CNS depressants, can be extremely dangerous5. Combining Xanax with opioids, for instance, can lead to severe sedation6 and a significantly higher risk of overdose deaths compared to opioids alone. Alcohol also enhances the effects of Xanax, increasing the risk of respiratory depression and life-threatening reactions.
Additionally, cannabis may elevate Xanax levels in the body, leading to increased side effects. Patients experiencing respiratory compromise from alprazolam overdose might require emergency airway management.
Avoiding mixing Xanax with other drugs and alcohol is crucial to prevent severe adverse effects and potential fatality.

Certain populations require special considerations when taking Xanax. In elderly patients:
For patients with hepatic impairment:
Gradual dosage reduction is crucial when discontinuing alprazolam to prevent withdrawal symptoms, especially for elderly patients.
Managing drug interactions is vital when using Xanax. Disclosing the following to healthcare providers helps manage the risks of mixing drugs:
This transparency helps prevent adverse effects and ensures the safe use of psychiatric medications.
Effectively managing side effects is crucial for those taking Xanax.
Key aspects include:
Relaxation techniques and counseling aid in coping with Xanax withdrawal symptoms. Combined with professional medical support, these strategies significantly reduce withdrawal discomfort and enhance treatment outcomes.
Bella Monte Recovery Center offers a drug and alcohol detox program in Desert Hot Springs CA. Located in Desert Hot Springs, California, our center provides tailored addiction treatments. Our holistic approach focuses on healing the root causes of addiction, not just the symptoms.
If you are struggling with Xanax dependence, we begin with medically supervised detox to manage withdrawal safely and comfortably. From there, our residential treatment program provides a structured, compassionate space for deep emotional healing, with individual therapy, trauma-focused care, and mental health support woven into every aspect of your stay.
We understand that every journey is different, so we create individualized treatment plans for each client. At Bella Monte, healing isn’t just about quitting but about rediscovering who you are without addiction.
Don’t wait. Call 888-964-5373 today to take the first step toward lasting recovery.
Xanax is primarily used to treat anxiety and panic disorders, effectively alleviating symptoms and fostering a sense of calm.
Common side effects of Xanax include drowsiness, dizziness, impaired coordination, and memory impairment, among others. It is important to monitor these effects and consult a healthcare professional if they occur.
Mixing Xanax with other CNS depressants, opioids, or alcohol significantly heightens the risks of severe sedation, respiratory depression, overdose, and potential death. Therefore, it is crucial to avoid these combinations to ensure safety.
Managing withdrawal symptoms from Xanax can be effectively accomplished by gradually tapering off the medication under medical supervision, alongside employing relaxation techniques, counseling, and regular check-ins with healthcare professionals.
Choosing Bella Monte Recovery Center for Xanax addiction treatment guarantees a holistic approach with personalized care in a structured environment, setting the foundation for lasting recovery. Our dedicated staff ensures you receive the support necessary to overcome your addiction effectively.
Navigating the complexities of Xanax use, side effects, and addiction treatment can be daunting. However, with the right knowledge and support, it is possible to manage these challenges effectively.
Understanding the uses, side effects, and risks associated with Xanax is crucial for safe and effective treatment.
Choose Bella Monte Recovery Center for comprehensive and supportive addiction treatment. Our holistic approach and specialized treatment plans provide the necessary tools for achieving long-lasting recovery. So, if you or a loved one needs help, don’t hesitate to reach out and take the first step towards a healthier future.
The content provided in this article is intended for general informational and educational purposes only and should not be construed as medical advice, diagnosis, or treatment.
Bella Monte Recovery Center™ does not provide clinical or medical recommendations via this article and does not assume liability for any reliance placed on the information herein. Xanax must only be administered under the direct supervision of a licensed medical professional. Do not start, stop, or alter any medical treatment based on this content without first consulting a qualified healthcare provider.
The mention of xanax or any other medication in this article does not imply endorsement or guarantee of results.
Reading this article does not establish a doctor-patient or provider-client relationship with Bella Monte Recovery Center™, nor does it constitute a formal medical evaluation. For professional help with benzodiazepine use disorder, please contact a licensed physician or call 888-964-5373 to speak with our admissions team. If you are experiencing a medical emergency, call 911 immediately.