Explore trauma mental health: from biology and PTSD to therapies like EMDR. Build resilience and heal today.
Understanding Trauma Mental Health and Its Impact
Trauma mental health refers to the psychological and emotional effects that result from experiencing or witnessing deeply distressing events. Understanding this connection is critical because trauma doesn't just affect your mind—it shapes how you function in daily life, impacts your relationships, and can lead to serious mental health conditions like PTSD, depression, anxiety, and substance use disorders.
Quick Answer: What You Need to Know About Trauma Mental Health
- Trauma is your reaction to an event, not the event itself—it causes lasting negative changes in how you think, feel, and function
- It affects everyone differently—no boundaries of age, gender, race, or socioeconomic status
- Your body responds automatically through fight, flight, freeze, flop, or fawn responses
- Common impacts include flashbacks, triggers, emotional numbing, hypervigilance, and difficulty trusting others
- It often co-occurs with depression, anxiety, dissociation, and substance use as coping mechanisms
- PTSD develops when symptoms last more than a month and significantly interfere with daily life
- Childhood trauma (ACEs) increases vulnerability to mental health issues and chronic diseases in adulthood
- Effective treatments exist, including trauma-focused therapies like CBT, EMDR, and trauma-informed care
- Recovery is possible with professional help, social support, and evidence-based treatment
Millions of people face the aftermath of traumatic experiences every day. Whether it's childhood abuse, a violent assault, a car accident, combat exposure, or even the accumulated stress of discrimination and systemic oppression, trauma leaves marks that can last for years.
Research shows that traumatic experiences are associated with both behavioral health and chronic physical health conditions, especially when they occur during childhood. In fact, a majority of adults have a history of childhood trauma and maltreatment. After major traumatic events like September 11, 2001, more than a quarter of New York residents who smoked cigarettes, drank alcohol, or used marijuana increased their consumption—demonstrating how trauma drives people toward unhealthy coping mechanisms. Additionally, mental health statistics for first responders highlight the profound impact of cumulative stressors on emotional well-being. This demographic often faces unique challenges, as their exposure to trauma can lead to higher rates of depression, anxiety, and PTSD compared to the general population. Understanding these statistics is crucial for developing tailored support systems that address the specific needs of those who serve on the front lines.
What makes trauma so complex is that it's not about the event itself—it's about how that event affects you. As one trauma survivor described: "I remember looking at pictures of myself around this time and I still feel you can see a fundamental change, the sparkle in my eyes just dims, it's almost as if the light of joy was snubbed out."
If you're reading this because you or someone you love is struggling with the effects of trauma, you're not alone. And importantly, trauma is treatable. With the right support and evidence-based care, healing is not just possible—it's achievable.

Defining Trauma and Its Reach
To understand trauma mental health, we first have to clear up a common misconception: trauma isn't just a "bad day" or a stressful week at the office. According to the APA Dictionary of Psychology, trauma is any disturbing experience that results in significant fear, helplessness, dissociation, or confusion. It is intense enough to have a long-lasting negative effect on a person’s attitudes and behavior.
At Bella Monte Recovery, we often explain to our clients in Desert Hot Springs that trauma is an injury. Just as a physical wound changes how you move your body, a psychological injury changes how you move through the world. It often challenges your view of the world as a safe, predictable, or just place.
Who is Affected by Trauma?
One of the most important things to realize is that trauma has no boundaries. It doesn't care about your bank account, your zip code in Southern California, your gender, or your race. While it is a universal human experience, research shows it is especially common among individuals struggling with mental health and substance use disorders. Finding effective trauma therapy options in California can be a crucial step in the healing process. With a variety of clinics and professionals offering specialized services, individuals are empowered to seek the help they need. These resources aim to create a supportive environment for recovery and personal growth.
Specific groups may experience trauma differently due to sociocultural contexts. For instance, what-are-microaggressions-and-how-are-they-a-form-of-trauma is a question that highlights how systemic issues like racism can create a state of chronic, "slow-burn" trauma. Whether it is a one-time event like a natural disaster or repeated exposure to trauma through domestic violence, the impact is deeply personal.
The Difference Between Stress and Traumatic Injury
We all deal with stress—the pressure of a deadline or a flat tire. But trauma is different. While everyday stress might make you irritable for an afternoon, a traumatic injury results in a fundamental change in functioning.
When we talk about trauma mental health, we are looking at an experience that overwhelms your ability to cope. Stress is something you "get through"; trauma is something that gets "stuck" in your nervous system. This "stuckness" is what leads to the negative changes in thinking and mood that characterize trauma-related disorders.
The Biology of Survival: How the Body Responds
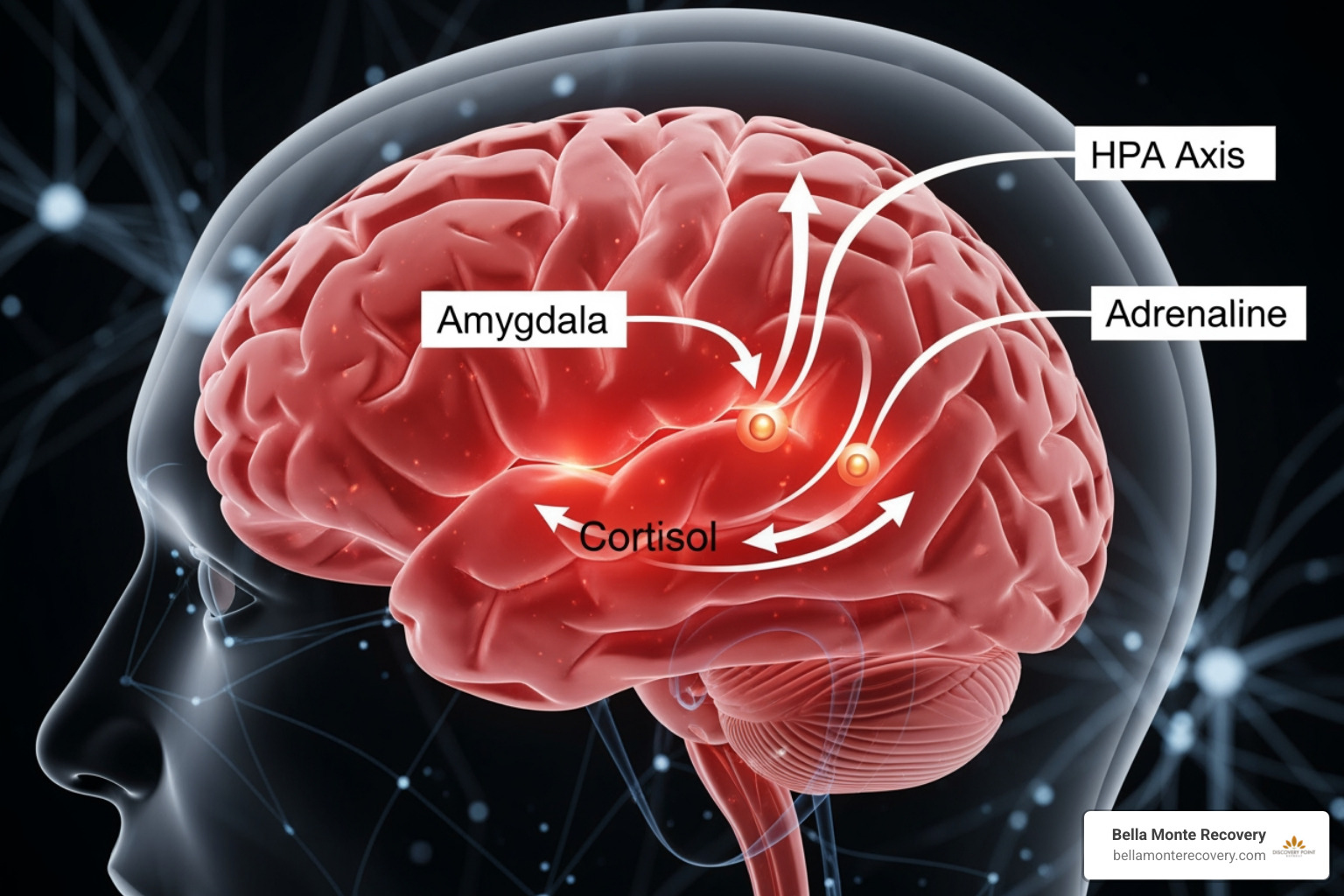
When you face a threat, your brain doesn't stop to ask for your opinion. The limbic system, particularly the amygdala, sounds the alarm. This triggers the HPA (hypothalamic-pituitary-adrenal) axis to flood your body with cortisol and adrenaline. This is a brilliant survival mechanism designed to keep you alive, but in cases of chronic trauma, this system stays "on" long after the danger has passed.
The physical effects of this biological hijacking include:
- Racing heart and sweating
- Digestive issues and stomach pain
- Chronic headaches and muscle tension
- Sleep disturbances and exhaustion
- Being easily startled (hypervigilance)
The Five Trauma Responses
Most people have heard of "Fight or Flight," but the body actually has a wider menu of survival strategies. We categorize these as the five "F" responses:
- Fight: Becoming aggressive or confrontational to overpower the threat.
- Flight: Physically or emotionally distancing yourself from the danger.
- Freeze: Becoming paralyzed or unable to act, like a deer in headlights.
- Flop: Becoming physically limp or unresponsive (common when physical resistance is impossible).
- Fawn: Trying to please or appease the person harming you to avoid further conflict.
Understanding these responses is vital for trauma mental health because it removes the element of shame. You didn't "choose" to freeze; your nervous system chose it for you to ensure your survival.
Managing Triggers and Flashbacks
A trigger is a sensory reminder—a smell, a sound, or even a specific tone of voice—that causes the brain to believe the trauma is happening right now. This can lead to a flashback, where you lose touch with the present moment and re-experience the event.
To manage these, we teach "grounding" techniques. These help engage the parasympathetic nervous system (the "rest and digest" system) to signal to the brain that you are safe. Recognizing-your-trauma-triggers-to-prevent-relapse is a core part of our work at Bella Monte, as it empowers you to stay in the present. Simple mindful breathing—inhaling slowly and exhaling longer than you inhale—is one of the most effective ways to tell your limbic system to stand down.
The Intersection of Trauma Mental Health and Co-occurring Disorders
Trauma rarely travels alone. Because the pain of trauma is so intense, many people develop other mental health challenges as a way to cope or as a direct result of a dysregulated nervous system. This is what we call "dual diagnosis" or co-occurring disorders.
| Experience | Normal Stress Reaction | Trauma-Related Disorder |
|---|---|---|
| Duration | Lasts a few days to weeks | Lasts more than a month |
| Daily Life | Able to function despite stress | Significant impairment at work/home |
| Intrusive Thoughts | Occasional worry about the event | Frequent, uncontrollable flashbacks |
| Avoidance | Avoiding the specific location | Avoiding people, places, and emotions |
Trauma Mental Health and Substance Use
There is a massive link between trauma mental health and substance misuse. When you are living with a brain that feels like it’s constantly under attack, it’s natural to want to "turn it off." This is the self-medication hypothesis.
Research shows that people who have experienced trauma are much more likely to increase their consumption of alcohol, tobacco, or drugs. For example, after the Oklahoma City bombing, residents reported double the normal rate of alcohol use. If you are struggling, you can find confidential advice on substance misuse to understand these risks. At Bella Monte, we treat anxiety and depression alongside trauma because you cannot effectively treat one without addressing the other.
Dissociation and Numbing
Dissociation is a mental "disconnection." It can feel like you are watching your life from a distance or that the world around you isn't real. While it starts as a protective mechanism to help you survive an overwhelming event, it can become a barrier to healing if it persists.
Similarly, emotional numbing—the inability to feel joy, sadness, or anything at all—is a common response. Some people may even develop symptoms that overlap with what-is-bpd (Borderline Personality Disorder), such as intense fears of abandonment or identity confusion, which are often rooted in early interpersonal trauma.
From ACEs to PTSD: Understanding Long-Term Impacts
The timing of trauma matters. The landmark Adverse Childhood Experiences (ACE) study proved that traumatic events in childhood—such as abuse, neglect, or household dysfunction—literally change the architecture of the developing brain.
As ACE scores increase, so does the risk for:
- Autoimmune and heart diseases
- Depression and suicide attempts
- Substance use disorders
- Difficulties with memory and concentration
When Trauma Becomes PTSD
Most people experience "acute stress" after a trauma, but for many, these symptoms resolve with time and support. However, when symptoms like intrusive memories, avoidance, and hypervigilance last for more than a month and interfere with your life, it may be diagnosed as ptsd.
According to the DSM-5, PTSD isn't just about "being jumpy." It involves a specific cluster of symptoms:
- Intrusion: Flashbacks, nightmares, or distressing memories.
- Avoidance: Staying away from reminders of the event.
- Negative Alterations: Persistent negative beliefs about oneself or the world, and emotional numbness.
- Arousal: Irritability, sleep problems, and a heightened startle response.
Complex PTSD and Intergenerational Effects
While standard PTSD often stems from a single event, Complex PTSD (C-PTSD) usually results from repeated, prolonged trauma, often involving interpersonal betrayal (like childhood abuse or domestic captivity). This can lead to deep-seated issues with emotional regulation and a fractured sense of self.
Interestingly, trauma can even be intergenerational. The stress of trauma can be passed down through parenting styles and even epigenetic changes, affecting children and grandchildren. In severe cases, untreated trauma can be misdiagnosed as other conditions, making it vital to distinguish between trauma-related symptoms and disorders like schizophrenia.
Pathways to Healing: Treatment and Resilience
The most important message we have for you is this: Trauma is not a life sentence. The brain possesses "neuroplasticity," meaning it can heal and form new, healthy connections. The APA recommendations for PTSD treatment highlight several evidence-based pathways to recovery.
Evidence-Based Therapies for Trauma Mental Health
We don't just use "talk therapy" for trauma; we use specialized interventions that address how trauma is stored in the brain and body.
- CBT (Cognitive Behavioral Therapy): Helps you identify and change the negative thought patterns (like "it was my fault") that trauma creates.
- EMDR (Eye Movement Desensitization and Reprocessing): A fascinating technique that uses bilateral stimulation (like eye movements) to help the brain "reprocess" traumatic memories so they no longer feel like they are happening in the present. You can learn more about emdr-therapy and how it facilitates healing.
- Psychodrama: This involves using role-play and guided drama to work through past events in a safe, controlled environment. Using psychodrama-to-resolve-trauma allows clients to gain new perspectives and "re-write" their internal narrative.
- Exposure Therapy: Gradually and safely facing the memories or situations you’ve been avoiding to reduce their power over you.
Building Resilience and Support Systems
Resilience isn't something you're born with; it's something you build. It involves prioritizing self-care, practicing mindfulness, and, most importantly, leaning on a support system.
Healing also involves addressing the "soul" of the person. This might mean learning how-to-heal-from-spiritual-trauma if your traumatic experience involved a breach of trust in a religious or spiritual community. Community resilience—knowing you are not alone in your struggle—is one of the most powerful predictors of long-term recovery.
Frequently Asked Questions and Conclusion
At Bella Monte Recovery Center in Desert Hot Springs, we see the incredible strength of the human spirit every day. We believe in a holistic approach to trauma mental health, addressing the mind, body, and spirit in a tranquil environment designed for renewal. Whether you are in Palm Springs or elsewhere in Southern California, our dual diagnosis services are here to help you reclaim your life.
What is the difference between PTSD and C-PTSD?
Standard PTSD usually follows a single, shocking event (like an accident). C-PTSD follows long-term, repeated trauma (like years of abuse). C-PTSD often includes additional symptoms like difficulty controlling emotions, feeling permanently damaged or "worthless," and severe challenges in maintaining relationships.
Can trauma cause physical health problems?
Absolutely. The constant flood of stress hormones can lead to cardiovascular disease, high blood pressure, chronic pain, and a weakened immune system. Trauma survivors often have higher rates of obesity, heart disease, and even a decreased life expectancy if the trauma remains untreated.
How can I support a loved one with trauma?
The best thing you can do is be present. Listen without judging or trying to "fix" them. Educate yourself about the biology of trauma so you don't take their irritability or withdrawal personally. Encourage them to seek professional help from a trauma-informed provider, but let them choose the timing whenever possible.
Recovery is a journey, not a destination. If you're ready to take the first step, we're here to walk beside you. Trauma may have changed your past, but it doesn't have to define your future.



